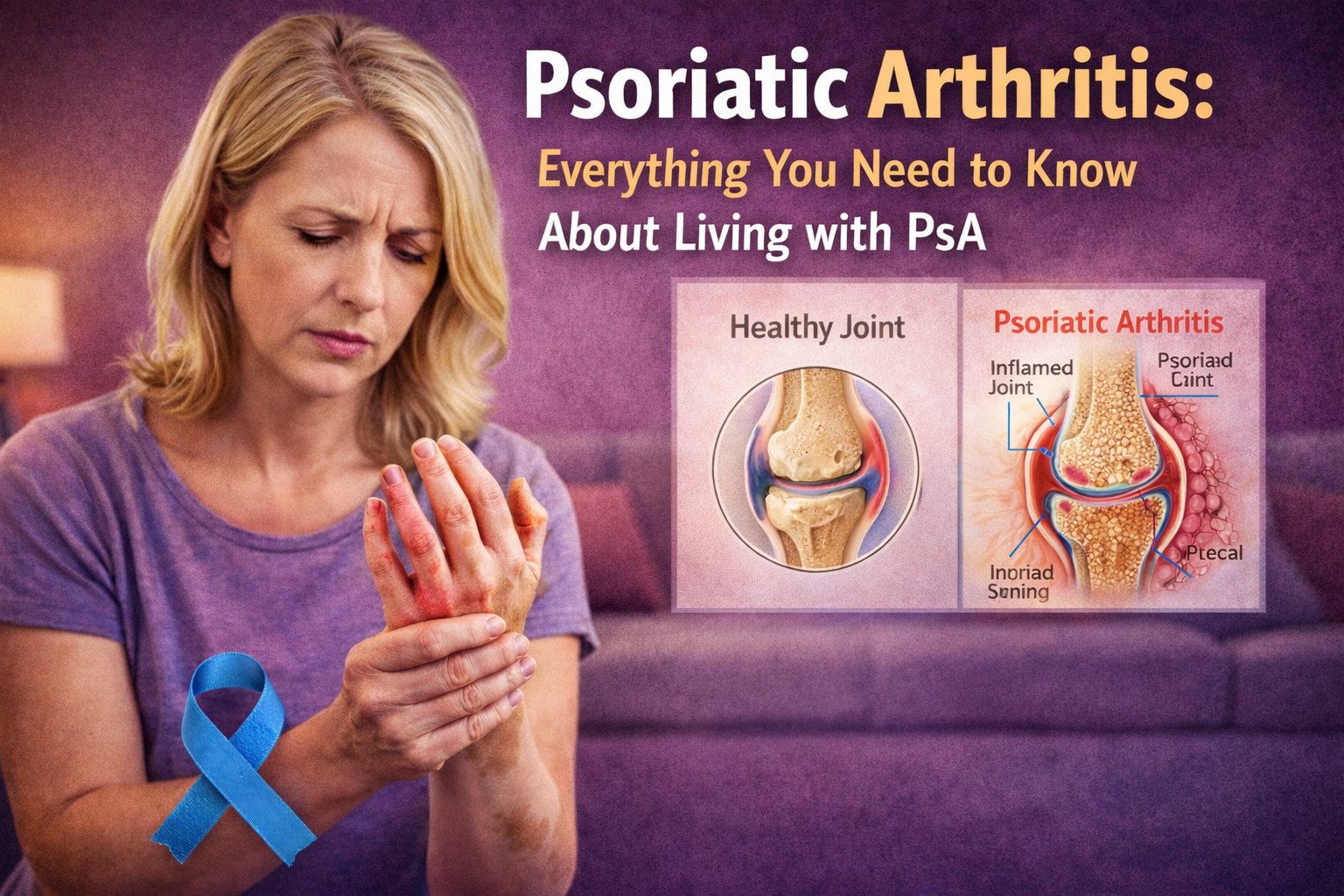
So you’ve got psoriasis, and now your joints are starting to hurt. Or maybe you’re dealing with joint pain and just discovered those scaly patches on your skin aren’t just dry skin. Welcome to the world of psoriatic arthritis, it’s not the club anyone wants to join, but you’re definitely not alone here.
Let’s break down what psoriatic arthritis really is, how it affects your body, and most importantly, how you can manage it and still live your best life.
What Exactly Is Psoriatic Arthritis?
Psoriatic arthritis (or PsA, as we’ll call it) is an autoimmune condition where your immune system gets confused and starts attacking your joints and skin. It’s like having an overenthusiastic security guard who can’t tell the difference between intruders and invited guests.
Most people with PsA have psoriasis first. Those red, scaly patches on your skin and then develop joint problems later. But here’s the kicker: about 15% of people get joint symptoms before any skin issues show up. Your body really knows how to keep you guessing, doesn’t it?
The Tell-Tale Signs You Shouldn’t Ignore
Joint Pain and Stiffness
This isn’t your regular “I worked out too hard” soreness. PsA joint pain tends to be worse in the morning or after you’ve been sitting for a while. Your fingers, toes, knees, ankles, and lower back are common targets. The stiffness can last for 30 minutes or longer, and it feels like your joints need a serious wake-up call before they start working properly.
Swollen Fingers and Toes
Ever heard of “sausage digits”? That’s the not-so-appetizing term doctors use when your fingers or toes swell up so much they look like little sausages. It’s called dactylitis, and it’s one of the hallmark signs of PsA. The swelling affects the entire digit, not just the joint.
Nail Changes
Your nails can tell a story too. Look for pitting (tiny dents), separation from the nail bed, discoloration, or crumbling. About 80% of people with PsA have nail problems. If you’ve been blaming your manicurist, it might be time to talk to your doctor instead.
Enthesitis
This fancy term means inflammation where tendons and ligaments attach to your bones. The most common spots are your Achilles tendon and the bottom of your feet. If you’ve got heel pain that won’t quit, this could be why.
Fatigue That Won’t Budge
We’re not talking about normal tiredness here. PsA fatigue is the kind that makes you feel like you’re walking through molasses, even after a full night’s sleep. It’s your body’s way of saying it’s working overtime fighting inflammation.
Types of Psoriatic Arthritis
PsA isn’t just one thing—it comes in different flavors, and knowing which type you have helps with treatment.
Symmetric PsA
This type affects the same joints on both sides of your body—like both knees or both wrists. It’s similar to rheumatoid arthritis and affects about 50% of people with PsA.
Asymmetric PsA
This one’s less predictable. It might hit your right knee and left wrist, without any pattern. It’s usually milder and affects fewer joints.
Distal Interphalangeal Predominant (DIP)
The joints closest to your fingernails and toenails are the main targets here. It often comes with nail changes too.
Spondylitis
When PsA goes after your spine and the joints connecting your spine to your pelvis, that’s spondylitis. You’ll feel stiffness and pain in your neck, lower back, and sometimes your hips.
Arthritis Mutilans
This is the rare but severe form that can actually deform and destroy joints, particularly in your hands and feet. The good news? It only affects about 5% of people with PsA, and early treatment can prevent it from getting this far.
Getting the Right Diagnosis
Here’s the frustrating part: there’s no single test that screams “You have PsA!” Your doctor will piece together the puzzle using several clues.
What Your Doctor Will Look For
They’ll examine your joints, check your skin and nails, and ask about your family history (PsA loves to run in families). Blood tests can rule out other types of arthritis and check for inflammation markers. X-rays, MRIs, or ultrasounds show what’s happening inside your joints.
Don’t be surprised if diagnosis takes time. On average, it takes about 2-3 years from when symptoms start to get a proper diagnosis. That’s way too long, which is why speaking up about your symptoms is so important.
Treatment Options That Actually Work
The goal isn’t just to ease your pain—it’s to stop the disease from damaging your joints permanently. Here’s what’s in your treatment toolkit.
NSAIDs: The First Line of Defense
Over-the-counter pain relievers like ibuprofen or naproxen can help with mild symptoms. They reduce inflammation and pain, but they won’t stop the disease from progressing. Think of them as temporary relief, not a long-term solution.
Disease-Modifying Antirheumatic Drugs (DMARDs)
These are the heavy hitters. Methotrexate is the most commonly prescribed DMARD for PsA. It slows down your immune system to reduce inflammation and prevent joint damage. You’ll need regular blood tests to make sure your liver’s handling it okay, but for many people, it’s a game-changer.
Biologic Medications
If DMARDs aren’t cutting it, biologics are your next step. These are targeted therapies that block specific parts of your immune response. TNF inhibitors (like Humira, Enbrel, or Remicade) are often the first biologics prescribed. Then there are IL-17 inhibitors and IL-23 inhibitors that target different inflammatory pathways.
Yes, they’re expensive. Yes, they’re usually injections or infusions. But they can literally stop joint damage in its tracks.
JAK Inhibitors
These are the newer kids on the block—pills that block enzymes called Janus kinases. They work fast and don’t require injections, which is a nice bonus. Your doctor might suggest these if biologics aren’t working or if you’d prefer an oral medication.
Corticosteroids
Steroid injections directly into painful joints can provide quick relief for flare-ups. They’re not a long-term solution because of side effects, but they’re great for getting through rough patches.
Topical Treatments for Your Skin
Don’t forget about treating the psoriasis part of PsA. Medicated creams, ointments, and light therapy can help manage your skin symptoms and might even help your joints feel better too.
Lifestyle Changes That Make a Real Difference
Medication is crucial, but what you do every day matters just as much.
Keep Moving (Even When You Don’t Want To)
I know, I know—exercise is the last thing you want to do when your joints hurt. But gentle, regular movement actually helps. Swimming, water aerobics, walking, and yoga are all excellent choices. They keep your joints flexible, strengthen the muscles around them, and help fight fatigue.
Just remember to listen to your body and rest when you need to. There’s a difference between pushing through discomfort and ignoring pain signals.
Watch Your Weight
Extra pounds mean extra stress on your joints, especially your knees, hips, and feet. Losing even 5-10% of your body weight can significantly reduce inflammation and pain. Plus, it lowers your risk of other conditions that often come with PsA, like heart disease and diabetes.
Eat an Anti-Inflammatory Diet
Load up on fruits, vegetables, whole grains, fish rich in omega-3s, nuts, and olive oil. These foods fight inflammation from the inside out. On the flip side, cut back on processed foods, red meat, sugar, and alcohol—they all promote inflammation.
Quit Smoking (If You Haven’t Already)
Smoking makes PsA worse, period. It increases inflammation, reduces the effectiveness of medications, and raises your risk of complications. If you’re struggling to quit, ask your doctor about support programs.
Manage Your Stress
Stress can trigger PsA flares. Find what works for you—meditation, deep breathing, therapy, hobbies, time in nature—and make it a non-negotiable part of your routine.
Protecting Your Joints Daily
Little changes in how you do everyday tasks can spare your joints a lot of grief.
Use larger, stronger joints when possible. Carry groceries with your forearms instead of gripping handles with your fingers. Open jars with a jar opener. Use electric can openers and kitchen tools. Get a shower chair if standing is painful. Choose shoes with good support and avoid high heels.
These aren’t signs of weakness—they’re signs of wisdom.
What About Flare-Ups?
Even with the best treatment, flare-ups happen. You’ll learn to recognize your triggers over time—maybe it’s stress, weather changes, overdoing it physically, or missing medications.
When a flare hits, rest the affected joints, apply ice or heat (whichever feels better), take your prescribed medications as directed, and don’t try to power through. Call your doctor if the flare is severe or lasting longer than usual.
The Emotional Side Nobody Talks About
Living with chronic pain and fatigue is exhausting, not just physically but mentally too. It’s completely normal to feel frustrated, angry, sad, or anxious about PsA. You might grieve the life you had before diagnosis, and that’s okay.
Don’t try to tough it out alone. Talk to a therapist, join a support group, or connect with others online who get it. Your mental health is just as important as your physical health.
Regular Monitoring Is Essential
PsA doesn’t just affect your joints and skin. It increases your risk of other conditions like cardiovascular disease, diabetes, depression, and inflammatory bowel disease. That’s why regular check-ups with your rheumatologist and primary care doctor are crucial.
You’ll need blood tests to monitor inflammation and medication side effects, imaging tests to track joint damage, and screenings for related conditions. Stay on top of these appointments—they’re catching problems before they become bigger problems.
Working with Your Healthcare Team
Your rheumatologist is the quarterback, but you need a whole team. A dermatologist for your skin, a physical therapist to keep you moving, a primary care doctor for overall health, and maybe a mental health professional too.
Be honest about what’s working and what’s not. If a medication isn’t helping or the side effects are unbearable, speak up. If you can’t afford your medications, tell them—there are often assistance programs available.
The Future Looks Brighter
Research into PsA is moving fast. New medications are being developed, and we’re learning more about what causes PsA and how to treat it more effectively. Early diagnosis and aggressive treatment can now prevent most people from developing severe joint damage.
You’re not destined for a wheelchair or a life of constant pain. With the right treatment and self-care, most people with PsA can live full, active lives.
Conclusion
Psoriatic arthritis is challenging, there’s no sugarcoating that. But it’s also manageable. With the right medications, lifestyle changes, and support system, you can keep this disease from calling all the shots in your life. Stay proactive about your treatment, listen to your body, and remember that bad days don’t last forever. You’ve got this.