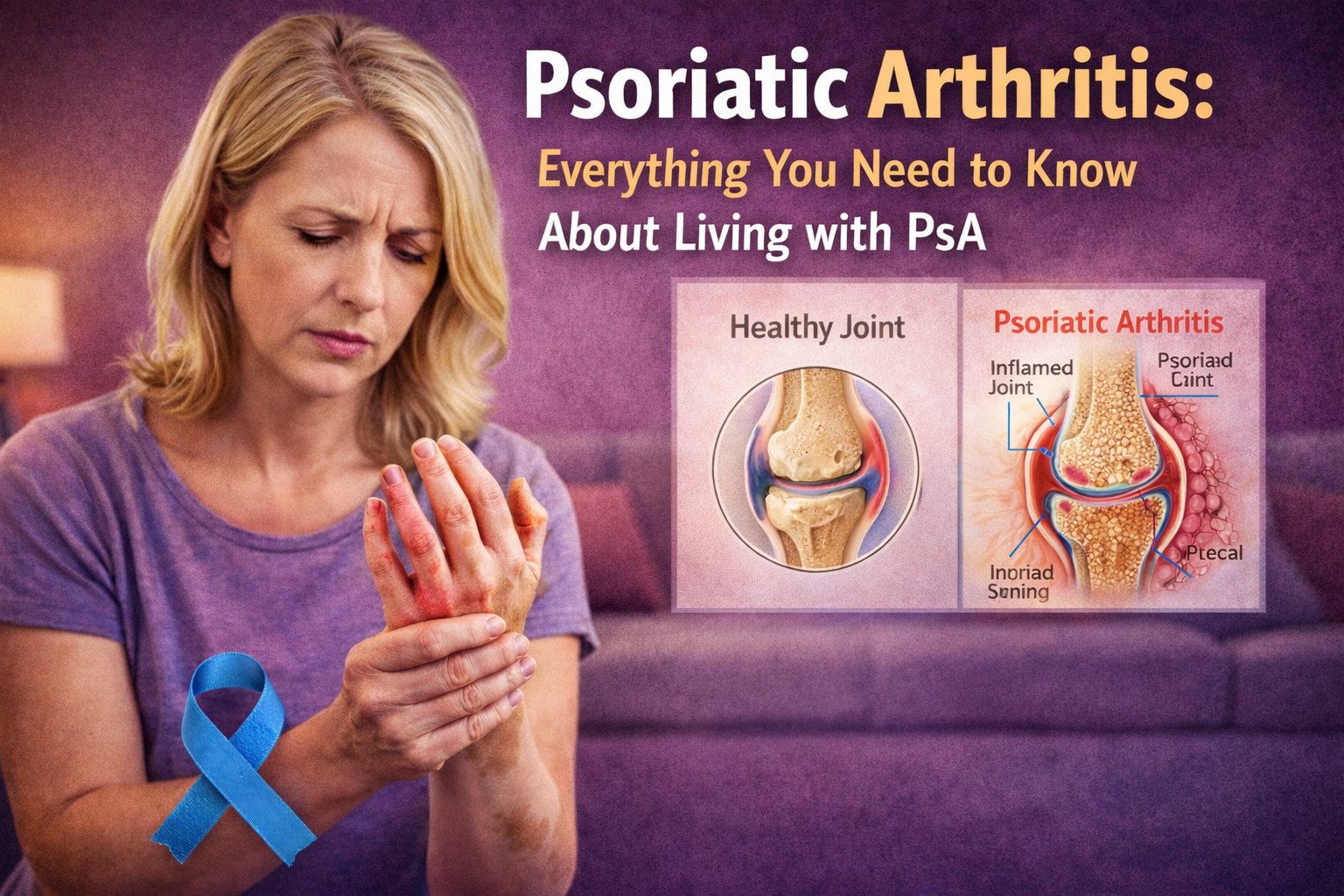
Bipolar disorder diagnosis involves a detailed assessment of mood episodes and behaviour patterns. It requires identifying specific symptoms, differentiating between types of bipolar disorder, and ensuring that the diagnosis is precise to guide effective treatment.
Symptoms and Clinical Presentation
Bipolar disorder is marked by episodes of mania or hypomania and episodes of depression. Manic episodes show elevated mood, increased energy, reduced need for sleep, and impulsive behaviour. Hypomania shares similar symptoms but is less severe and doesn’t cause major impairment.
Depressive episodes include low mood, loss of interest, fatigue, and difficulty concentrating. These symptoms cause significant distress and affect daily functioning. Psychiatrists evaluate the duration, intensity, and impact of these episodes to determine if they meet diagnostic criteria.
Mood changes in bipolar disorder are distinct from typical mood swings and must last for a specific period. Rating scales and clinical interviews help in capturing the pattern and severity of symptoms.
Types of Bipolar Disorder
There are mainly two recognised types: Bipolar I and Bipolar II disorder. Bipolar I involves at least one manic episode, which may be followed by depressive episodes. A manic episode is severe and can require hospitalisation.
Bipolar II involves at least one hypomanic episode and one major depressive episode. Hypomanic episodes are milder but still represent a clear change in mood and activity levels.
Other subtypes, like cyclothymia, involve less severe but chronic mood fluctuations. Correctly identifying the subtype is important for treatment planning.
Importance of Accurate Diagnosis
Accurate diagnosis reduces the risk of mistreatment, which can worsen symptoms. Bipolar disorder is often confused with unipolar depression because depressive episodes are common to both.
Misdiagnosis can delay effective treatment for years, increasing risks such as suicide and other health problems. Clinicians use structured interviews, mood charts, and medical history review to improve accuracy.
Early and correct diagnosis allows clinicians to tailor therapies like mood stabilisers and psychotherapies, improving long-term outcomes. It also helps in managing coexisting conditions, which are common in bipolar disorder.
Key Diagnostic Criteria and Standards
Bipolar disorder diagnosis depends on clear criteria and guidelines to ensure accuracy. Healthcare professionals use recognised manuals and careful evaluation to distinguish bipolar disorder from other conditions with similar symptoms.
DSM-5 Criteria
The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) defines bipolar disorder by specific mood episodes. For Bipolar I, a person must have experienced at least one manic episode, which includes an elevated or irritable mood and increased activity or energy lasting at least one week.
Bipolar II requires a hypomanic episode lasting at least four days, along with a major depressive episode. Hypomania is a less severe form of mania without significant impairment.
Both types require symptoms not better explained by another mental health condition. The DSM-5 also includes criteria for mixed episodes and rapid cycling.
ICD-11 Guidelines
The International Classification of Diseases, 11th Revision (ICD-11) uses a similar approach, focusing on mood episodes. It groups bipolar disorder under mood (affective) disorders and details the duration and severity of manic and depressive episodes.
ICD-11 emphasises the importance of observing episodic mood changes that cause clear functional impairment. It also notes the need to exclude other causes, such as medical conditions or substance use.
This classification is widely used globally and supports diagnosis alongside the DSM-5.
Differentiating Bipolar Disorder from Other Conditions
Diagnosis involves ruling out other mental health issues with overlapping symptoms. For example, unipolar depression can look like bipolar depression but does not include manic or hypomanic episodes.
Conditions like schizoaffective disorder and some personality disorders may show mood swings but have distinct features such as psychosis or personality traits.
Clinicians must assess symptom patterns, duration, and effects on daily life. They often use patient history, reports from family, and sometimes mood charts to confirm bipolar disorder accurately.
Essential Assessment Methods
Diagnosis of bipolar disorder involves careful examination of mood patterns, behaviours, and medical history. Several key methods help clinicians gather the necessary information to identify the disorder accurately.
Comprehensive Patient Interview
The interview is central to assessing bipolar disorder. The clinician asks detailed questions about mood changes, including periods of mania, hypomania, and depression. Patients describe symptoms, their duration, and how these affect daily life.
The interview also explores behaviours such as sleep patterns, energy levels, and impulsive actions. It aims to rule out other causes for mood changes, like substance use or medical conditions.
Accurate self-reporting is critical. Sometimes, family members provide additional details. Structured interview tools may be used to ensure all relevant symptoms are covered.
Psychiatric Evaluation
A psychiatric evaluation provides a professional assessment of mental health. It often uses standard diagnostic tools based on criteria from resources like the DSM-5-TR.
The clinician evaluates mood episodes to distinguish bipolar disorder from similar conditions, such as major depression or borderline personality disorder. This includes checking for manic or hypomanic episodes.
Assessment also considers current mental status, cognitive function, and risk factors. This helps clarify diagnosis and guides treatment planning.
Family and Medical History Review
Family history plays an important role because bipolar disorder can run in families. The clinician asks about relatives with mood disorders or other mental illnesses.
Medical history is reviewed to exclude physical illnesses that might mimic bipolar symptoms. This may include thyroid problems or neurological disorders.
A history of past treatments, hospitalisations, and responses to medication informs diagnosis and management decisions. This review helps provide a fuller picture of the patient’s condition.
Psychological and Physical Tests for Bipolar Disorder
Diagnosing bipolar disorder involves several tests. These include questionnaires to assess mood patterns, cognitive evaluations to check brain function, and medical exams to rule out other causes. Each type of test provides specific information to help confirm the diagnosis.
Mood Questionnaires and Self-Reports
Mood questionnaires are commonly used tools for identifying symptoms of bipolar disorder. They ask the individual about experiences of mood swings, changes in energy, sleep, and behaviour.
These questionnaires often include standardised scales like the Mood Disorder Questionnaire (MDQ). Patients report the frequency and severity of mood episodes, which helps clinicians distinguish between bipolar disorder and other mood disorders.
Self-reports are important because they offer insight into the patient’s experience over time. However, these tools are not foolproof and work best when combined with clinical interviews and observations.
Cognitive and Neuropsychological Testing
Cognitive testing measures memory, attention, and problem-solving abilities. For bipolar disorder, these tests can reveal difficulties that might occur during mood episodes or in between them.
Neuropsychological assessments help determine if there are patterns of brain dysfunction linked to bipolar disorder. For example, reduced executive function or slower processing speed may be noted.
These tests are not used alone to diagnose bipolar disorder. Instead, they support the overall evaluation by adding detail about how the condition affects thinking and behaviour.
Laboratory and Medical Examinations
Lab tests and physical exams check for medical conditions that may mimic or worsen bipolar symptoms. Blood tests often include thyroid function, blood count, and chemistry panels.
Urine toxicology screens for substance use that could affect mood. Sometimes, thyroid problems or other illnesses cause mood changes similar to bipolar disorder.
These examinations are vital as they ensure that the diagnosis is accurate and guide proper treatment by ruling out physical health issues.
Challenges and Considerations in Diagnosis
Diagnosing bipolar disorder is complex due to overlapping symptoms with other conditions and variations caused by cultural and age differences. These factors affect how symptoms are reported and interpreted, leading to difficulties in reaching an accurate diagnosis.
Misdiagnosis and Co-Occurring Disorders
Bipolar disorder is often misdiagnosed because its symptoms can resemble other mental health conditions. For example, depressive episodes may be mistaken for major depression, while manic symptoms can be confused with anxiety or personality disorders.
Co-occurring disorders, such as substance abuse or anxiety, complicate diagnosis further. These conditions may mask bipolar symptoms or alter their presentation, making it harder for clinicians to identify the correct illness.
Clinicians rely on detailed interviews to distinguish bipolar disorder from similar conditions by examining symptom patterns, duration, and impact on functioning. Despite this, the average delay in diagnosis ranges from 5 to 10 years, which can delay appropriate treatment.
Cultural and Age-Related Factors
Cultural background influences how patients express symptoms and their willingness to seek help. Some cultures may view mood changes differently, affecting symptom reporting and clinician interpretation.
Age also affects diagnosis. Children and adolescents may show mood shifts that differ from adults, often leading to confusion with behavioural or developmental disorders. Older adults may have co-existing medical issues that interfere with diagnosis.
Rapid cycling of mood episodes within a year creates additional challenges across all age groups. Awareness of these variations is essential for accurate assessment and tailored treatment plans.
FAQs
What is the main method for diagnosing bipolar disorder?
Diagnosis is based on a clinical assessment of symptoms, mood episodes, and medical history. There are no blood tests or scans that can confirm the disorder.
Can bipolar disorder be diagnosed in children and teenagers?
Yes, but symptoms in young people may look different from adults. Their mood changes might not fit neatly into standard categories.
How do doctors tell the difference between bipolar disorder types?
They assess the pattern and severity of mood episodes. Bipolar I involves full manic episodes, while Bipolar II includes hypomanic episodes and depression.
Are there any tests for bipolar disorder?
There are no definitive tests. Doctors rely on interviews and observation. They also rule out other conditions like brain injury or medical illnesses that could cause mood changes.
Why is bipolar disorder sometimes misdiagnosed?
Symptoms such as mild hypomania can be overlooked. People often report more depressive symptoms, which leads to confusion with other mood disorders.
What do doctors consider during assessment?
They look at:
- History of mood changes
- Family history of mental illness
- Duration and impact of symptoms
All of these help to meet the criteria set out in the DSM-5.